
EyePromise - Upgrade Your Eyes
EyePromise provides vitamins, technology, and support to enhance and protect vision for life.

Who We Are
EyePromise provides eye health nutraceuticals, technology, and support for eye care professionals.

Our Mission
Innovate and market premium, efficacious, science-based vitamins, technology and support to preserve and enhance eye health globally.

Our Values
We value science, quality, results, transparency, and most importantly, your dedication to eye health.
Solutions For Doctors
Whatever your patients need, we’ve got them covered. Learn more about our eye health nutraceutical solutions.
Supporting Doctors Everywhere
Through years of research, we discovered the impact key nutrients have on all aspects of sight. We saw the need for a nutrition solution and we created one. EyePromise is an entire line of eye health and visual performance products, each with a focus on specific conditions and outcomes.
Become a part of the EyePromise network to join doctors across the country helping their patients see better and react faster.
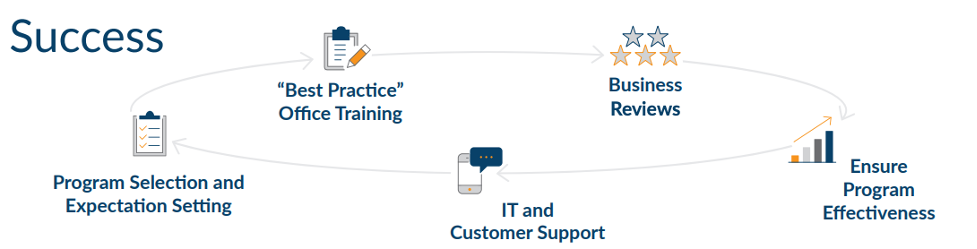
Partnership:
-
Ensuring patient and financial value for the practice and doctor.
-
Dedicated “team” approach to train, coach, and provide ongoing assistance to doctors, groups, and staff.
-
Conduct practice observation sessions to continually develop and refine best practices with data.

Eye Care Professional, Chicago, IL

Professor, Pacific University Oregon

Professional Golfer
**Endorsements may be in exchange for product and/or compensation.

**Endorsements may be in exchange for product and/or compensation.














